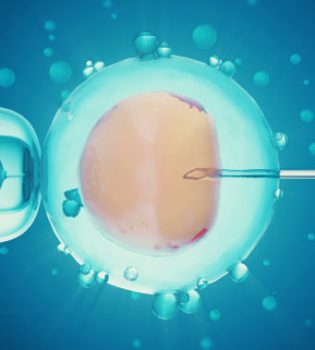
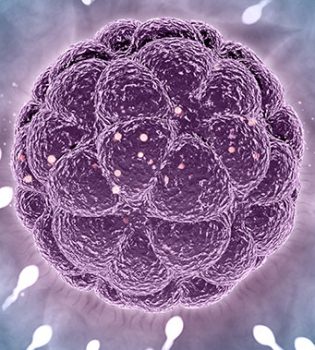
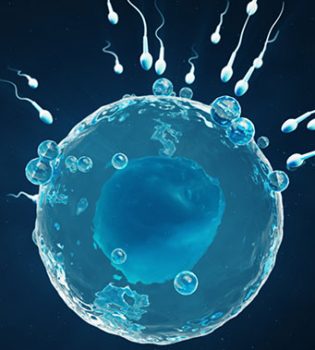
Male infertility is the cause of about half of the couples who do not have children in the society. In other words, the male factor may be a problem in approximately half of infertile couples. It may be necessary to start treatment without waiting in cases such as male-related cases such as azoospermia (no sperm), retrograde ejaculation, and in cases such as female age factor. The ICSI method allowed men to have children even if there was no sperm in their semen. However, performing this procedure requires the presence of sperm production in the testicles of the patient, even if just a bit. In other words, sperms must be obtained from the testicles of the patient. Obtaining sperm from the testicles is performed by applying different methods according to the patient’s condition. Testicular biopsy can be performed in men with no sperm detected in semen analysis. With this procedure, the reason for the absence of sperm is revealed. In other words, it is revealed with this method whether it is not seen in the semen because sperm cannot be made or because there is a blockage. In cases with severe impairment in sperm production, TESE is a method used to find small sperm-producing foci inside the testicle. The presence of sperm is investigated by taking pieces of a few millimeters from several foci from the testicle. Microtese is the process of finding sperm from the tubes in which sperm are produced under the microscope. With this method, there is a 36%-68% chance of finding sperm in cases not related to obstruction, that is, in cases with problems in sperm production. With the microtese method, the chance of finding sperm in each biopsy increases with less testicular tissue. In other words, this chance is higher than the classical TESE procedure. In addition, another advantage is that it minimizes vascular injuries in the testicular tissue area during biopsy and helps the embryologist to find sperm more easily in small pieces.
How long does the patient have to rest after Microdissection tese?
After the operation, the patient is sent home after being kept under observation for 2-3 hours as he receives general anesthesia. Dressing and control are carried out 2 days after the procedure. It is recommended to avoid excessive physical activity, long journeys, and long-term driving for an average of 7 days. No sexual activity for 15 days.

Is General Anesthesia Used in Sperm Collection by Surgical Method?
Sperm retrieval from the testicle can be performed in two ways, under local and general anesthesia. Applications performed under local anesthesia are to obtain sperm from the testicle with a needle (PESA-TESA) or to remove testicular tissue with a small incision (TESE). These methods are the methods that can be chosen when it is sure that sperm is produced in the testis and there is no sperm in the semen due to obstruction. In our center, the procedure of Microdissection TESE (finding sperm from the testicle) is performed under microscope for patients with sperm production disorder in the testicle and no sperm in the semen. General anesthesia is used in the operation performed with this method. General anesthesia is preferred because it is difficult for the patient to lie still for a long time with local anesthesia when the operating microscope is used. The operation performed under the guidance of a microscope has many advantages over the previously applied local multiple testicular biopsy method. With the operation microscope, the structures in the testicles are examined in detail at x20 magnification, and samples are collected from the areas where sperm is produced. During the testicular incision, the areas with less vascularity are selected with the microscope and the incision is made, which reduces the bleeding that will occur during the operation. In addition, it provides the protection of the vascular structure that feeds the testicle. Since very little tissue is removed (70 times less than a multiple biopsy), it does not cause a decrease in the testosterone hormone level in the blood.
The Importance of Genetic Analysis in Male Infertility
In recent years, advances in the field of genetics have enabled us to obtain very important information about the causes of male infertility. Deletions in the genes on the Y chromosome from the sex chromosomes lead to a situation such as decreased sperm production or no sperm production in the testicle, although the body structure and functions are normal. Likewise, in genetic diseases caused by numerical abnormalities in sex chromosomes (for example, the most common 47 XXY Klinefelter syndrome), testicular development may be insufficient and sperm production may be decreased. In addition, if the ducts carrying sperm from the testicles are not existing congenitally, although there is normal sperm production in the testis, sperm cannot be seen in the semen because there is no way out. This is genetically linked to a disease called Congenital Bilateral Vas Deferens Agenesis (CBAVD).